The heart transplant
Patients who are on the waiting list for a donor heart are closely monitored by their transplant center during the entire waiting period. Regular examinations are carried out to check their state of health and medication is adjusted if necessary. Patients are also trained on post-op medication and hygiene measures. Another important component is physical preparation for the transplant through strength exercises and physiotherapy (known as prehabilitation).
As soon as a suitable donor heart is available, the transplant center informs the patient immediately. He or she is immediately prepared for the operation at the hospital. The transplantation itself is a complex procedure lasting several hours. This is followed by post-operative care in the hospital and finally aftercare.
Prehabilitation
Physical fitness
Physical preparation for transplantation, also known as prehabilitation, is of crucial importance for the success of the treatment. The fitness of patients before the procedure has a direct influence on the post-operative prognosis. Physical fitness also plays a role in the urgency rating for a donor organ.
In many cases, rehabilitation therefore also makes sense during the evaluation process.
It is recommended to take part in a cardiac sports group or a heart failure group and to take advantage of regular physiotherapy. Online cardiac exercise classes can be a useful addition to this.

In addition, strength exercises are recommended several times a week, which are taught by physiotherapists and then carried out independently. Muscle strength and mass in particular contribute to an improved prognosis after the operation.
Weight and diet
In the event of excessive weight loss and the development of underweight (pulmonary cachexia), nutritional therapy with counseling and high-calorie supplementary food may be recommended.
In the case of obesity, dietary or pharmacological treatment is recommended. Ideally, the body mass index (BMI) should be between 22 and 25 kg/m².
Psyche
If patients suffer from panic attacks or develop an adjustment disorder (often with recurring shortness of breath and thus fear of death), they should receive psychological treatment. Fears often lead to withdrawal and thus to insufficient physical activity.
Admission and preparation for surgery
To ensure that listed patients can be informed at any time as soon as a suitable donor heart is available, they should have a German residence and accessibility regulation. For stays outside Germany, patients must be temporarily NT-listed (not transplantable).
Once brain death and the deceased's willingness to donate have been determined by the DSO at the donor hospital, Eurotransplant will be informed of the available organ.
The foundation, which is based in the Netherlands, then determines which recipient is most suitable and notifies the transplant center where the patient is being treated.
There, a surgeon checks the medical data provided by the donor organ. If he or she decides to accept it, a specialized team of doctors sets off for the donor hospital.
Once the team has arrived at the donor center, it takes over the removal of the organ. This is the start of the ischemia period, during which the organ is not supplied with blood. This must be kept as short as possible to avoid damaging the organ.
At the same time as the organ is removed, the recipient is prepared for the transplant in the operating theater. Final preliminary examinations take place.
When the removal team makes its way back, the operation begins. This ensures that the ischemia time can be kept as short as possible. In the case of donor hearts, for example, the ischemia time should not exceed four hours.
The ischemia time, during which the removed donor organ is not supplied with blood, must be kept as short as possible in order to avoid damaging the organ. It must not exceed four hours for donor hearts.
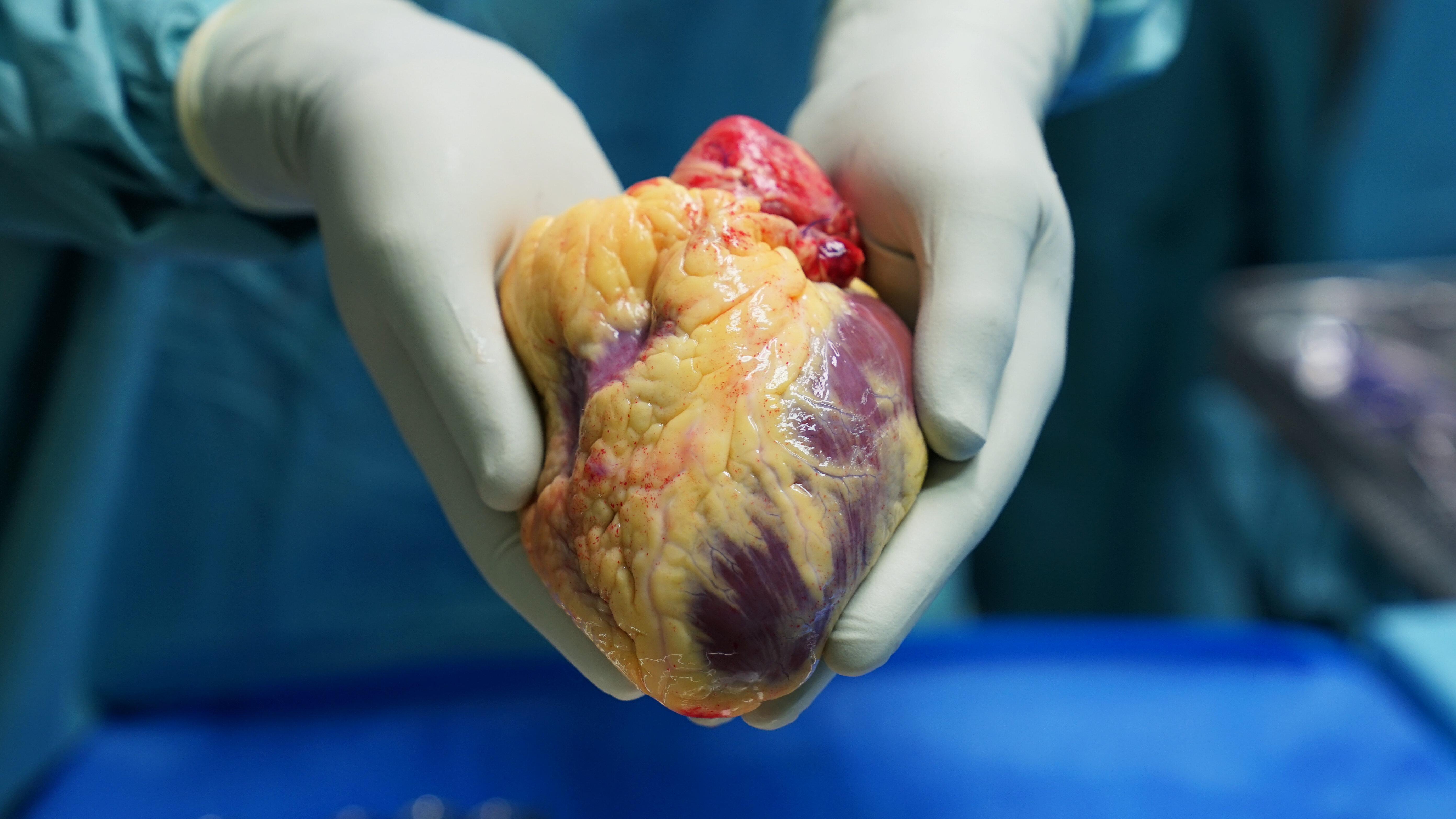
The transplant itself is performed under general anaesthetic and can take up to twelve hours.
The experienced surgical team works closely with the anaesthesiology and intensive care specialists.
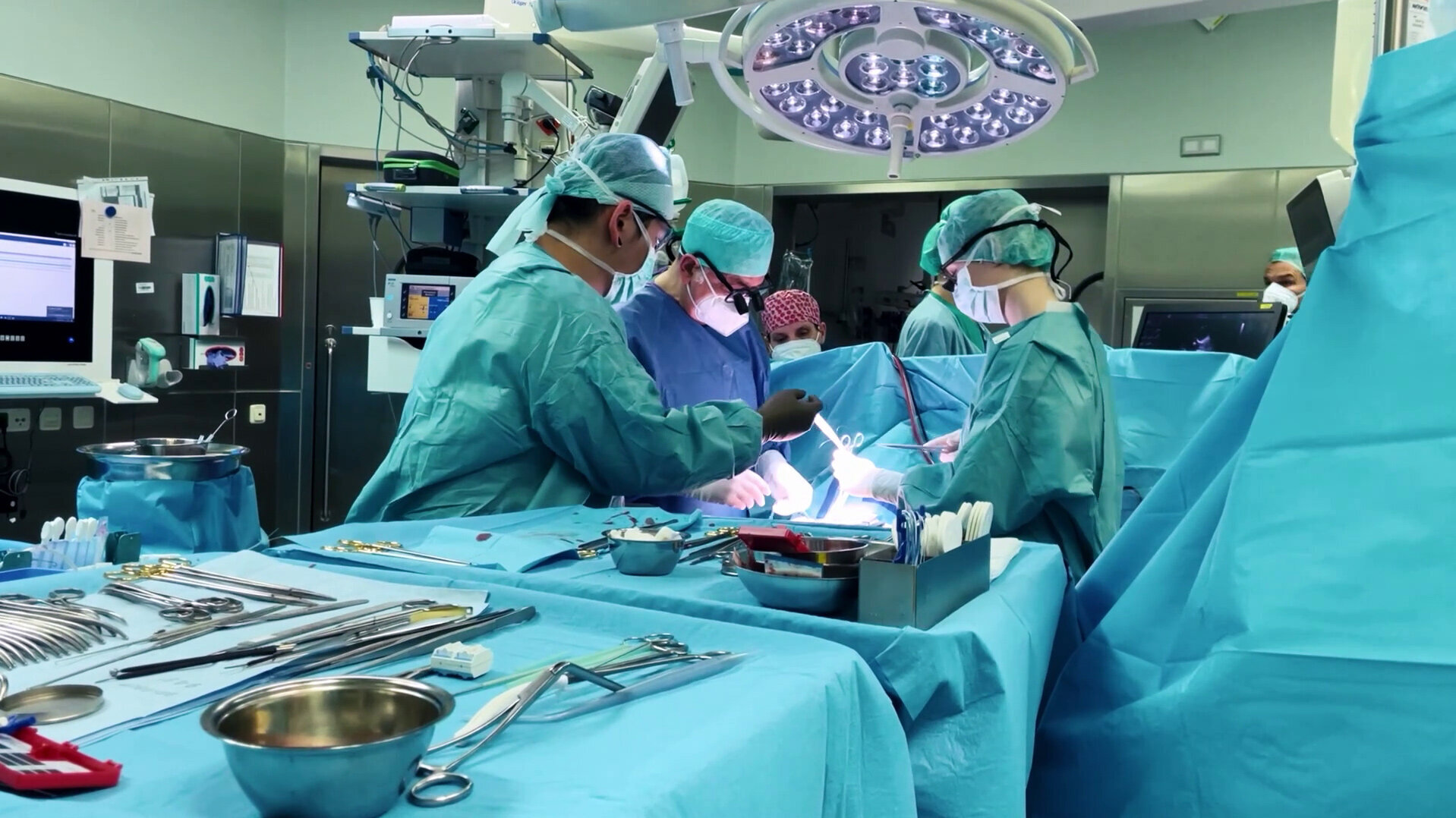
Firstly, the chest is opened to gain access to the heart. The patient is then connected to the heart-lung machine. This takes over the circulatory and oxygen supply because the patient's own heart is at a standstill during the operation.
The surgeon then cuts the large vessels and removes the diseased heart. The donor heart, which is stored in a special cool box, is then positioned in the body, gradually sewn into place and connected to the atria and arteries.
Once the donor heart is in place, the blood flow to the new organ is started. Warm blood flows through the heart again. Many donor hearts begin to beat on their own; sometimes a slight electrical impulse is required.
When the new heart is pumping steadily, the heart-lung machine is gradually reduced and finally switched off. The doctors check the organ for possible haemorrhaging.
The chest is then closed again.
Documentary ‘Gift of Life’
At the age of 37, our patient Franziska Bleis falls ill with myocarditis; her condition becomes increasingly critical. She finally receives a donor heart at the DHZC. We were allowed to accompany Franziska on her way back to life with the camera, including in the operating theatre. The result is a 25-minute documentary that aims to educate and encourage.
After the transplant
After the operation, patients are initially ventilated and anaesthetised in the intensive care unit WD1i. There they are monitored around the clock by doctors and nurses. During the operation and in the initial period afterwards, patients are artificially ventilated with a ventilator. As soon as they are able to breathe sufficiently on their own, the breathing tube is removed and the patients can eat independently again. On the ward, cardiac function, the circulatory situation, the wake-up reaction and possible rejection reactions are closely monitored. At the same time, patients are mobilised.
Immediately after the operation, physiotherapy care begins in the intensive care unit. Specialised breathing trainers and physiotherapists perform breathing and muscle training exercises with the patients.
As soon as their physical condition allows, patients are transferred to our transplant ward WD3. In most cases, they spend the time until rehabilitation on the heart failure and transplant ward, which is certified by the German Society of Cardiology (DGK). Under careful medical and nursing supervision, patients are prepared here for their discharge from hospital.
In order to check organ function, the team of doctors at the DHZC carries out numerous examinations on the patients in the first few weeks after the transplant. These include blood samples, X-rays, ECG and echocardiography. Before patients are discharged into rehabilitation , we carry out a cardiac catheterisation with a heart muscle biopsy and, if necessary, a cardiac MRI to rule out rejection of the donor organ.
Heart and lung transplant patients spend the first post-operative phase on ward WD3. The team also cares for long-term transplant patients who have to be hospitalised at the DHZC.

Risks and complications
Like any other operation, a heart transplant is also associated with risks. Complications can occur early on or only in the long term.
The risks include
- Complications after the operation: Immediately after the operation, post-operative bleeding or wound infections may occur.
- Initially, it may be necessary to supportkidney function with procedures such as dialysis. In the vast majority of cases, this provides temporary support.
- Acute rejection: The immune system recognises the donor heart as foreign and rejects it.
- Infections: Patients have to take medication for the rest of their lives after the transplant to suppress the immune system. This makes them more susceptible to infections and viral infections.
- Other side effects of immunosuppressants: The medication, which is intended to prevent rejection of the donor heart, can increase the risk of suffering from certain diseases such as high blood pressure or kidney dysfunction.
- Complications of the heart itself, such as cardiac arrhythmia or coronary artery disorders.
- Vascular and circulatory problems such as thrombosis or fluctuations in blood pressure.
- Psychological stress such as depression, fear of organ rejection or difficulties in adapting to the changed lifestyle.
Forecast
The average survival time after a heart transplant has risen steadily in recent years and will continue to rise in the future, mainly due to improved treatment methods.
Most people can return to many of their normal activities within a few months. A heart transplant therefore noticeably improves the quality of life of these patients.
The average survival time after a heart transplant is around 20 years, which is significantly longer than the average prognosis before the transplant, which is often in the region of months.
Of course, the prognosis is very individual from patient to patient and depends on many different factors. Above all, the transplant function (i.e. the ‘performance’ of the donor organ and possible complications after the transplant) as well as secondary diseases, age and personal lifestyle influence the actual survival time.
Another factor is the experience of the transplant centre: experienced, highly specialised facilities often achieve better results. The one-year survival rate at the DHZC is 87 per cent; the national average is 81 per cent. Three years after the operation, 83 per cent of heart transplant patients at the DHZC are alive - the national average is 72 per cent.
Video: Patient Mathias Schumann
Our patient Mathias Schumann has been suffering from heart failure for 10 years. When his condition deteriorates rapidly, he is connected to an artificial heart. Our doctors move the connection between the body and the pump from the groin to the collarbone - so our patient can stand up and move around. After a short wait, he survives the heart transplant very well. Today he is doing very well.
Rehabilitation
Rehabilitation after a heart transplant is a key component of recovery and long-term treatment success. It often begins shortly after the operation in hospital and continues in specialised rehabilitation centres or on an outpatient basis.
Rehabilitation is the phase of returning as fully as possible to private, social and professional life. An important part of this is targeted training to restore physical performance. But we also support our patients psychologically and emotionally during this time.
In detailed discussions, you will learn exactly
- what health risk factors there are and how you can avoid them,
- what the signs of organ rejection are,
- how you can protect yourself against infections,
- what social support options are available.
Rehabilitation in the rehabilitation clinic can begin,
- if there are no medical objections to your transfer
- if you are able to look after yourself again (e.g. washing and dressing)
- if you only need a little nursing help and are physically ready for rehabilitation training.
Depending on the course of the disease, this is usually the case around six to eight weeks after the transplant. As a rule, our patients are transferred to the Seehof Rehabilitation Centre in Teltow on the southern outskirts of Berlin directly after their inpatient stay at the DHZC. The centre has over thirty years of experience with transplant patients from our clinic. It is located in a green, quiet neighbourhood. You will be given a single room and can receive visitors or go on excursions. The journey to the DHZC only takes about 30 minutes, so you can be back at our clinic quickly in urgent cases.
How does the rehabilitation stay work?
- Physical activity such as bicycle ergometer training, muscle building on equipment, gymnastics in a group or individually with exercise therapists
- Passive applications such as lectures, counselling, individual and group training sessions
- Relaxation training and, if necessary, psychotherapeutic counselling
Medical rounds are held daily - including at weekends - so that complications can be recognised quickly and treated in consultation with the DHZC. Echocardiograms, ECGs and medication levels are also carried out regularly. The dosage of your medication will be adjusted if necessary. Invasive, stressful examinations are not usually necessary. During your stay, you will usually only have to visit the DHZC transplant outpatient clinic once.
What is the effect of rehabilitation?
Decades of experience and numerous studies have proven the considerable benefits of rehabilitation in improving physical and mental performance and quality of life. In addition, you will now be able to independently perform the necessary check-ups (e.g. measurement of blood pressure, pulse, fever and weight), you will know how to behave correctly at home and you will recognise the signs of possible complications.
Aftercare and support
We remain at your side even after the transplant. Long-term, lifelong aftercare includes:
- regular check-ups in our transplant outpatient clinic
- lifelong medical treatment to prevent rejection reactions and infections
- the support with reintegration into everyday life
- Training in dealing with the new organ, hygiene measures, etc.
- transplantation-appropriate nutritional counselling
- The advice and contact mediation to training programmes and physiotherapy
Detailed information on aftercare and support at the DHZC can be found on the page Care for heart transplant patients.
Progress in heart transplantation
Systems for organ preservation
At the DHZC, we use a novel system for the preservation of donor hearts , which enables better organ function and longer transport times whereby the organ is supplied with a special nutrient and preservative fluid via a pump during transport. The new technology should enable even better function of the donor organs and significantly longer transport times. The donor pool is also expected to expand, because more donor organs could be accepted that previously had to be rejected because they would not survive transport.
After extensive testing, the system was approved for use in humans as part of an international study and will be used for the first time in Germany at the DHZC in autumn 2021.
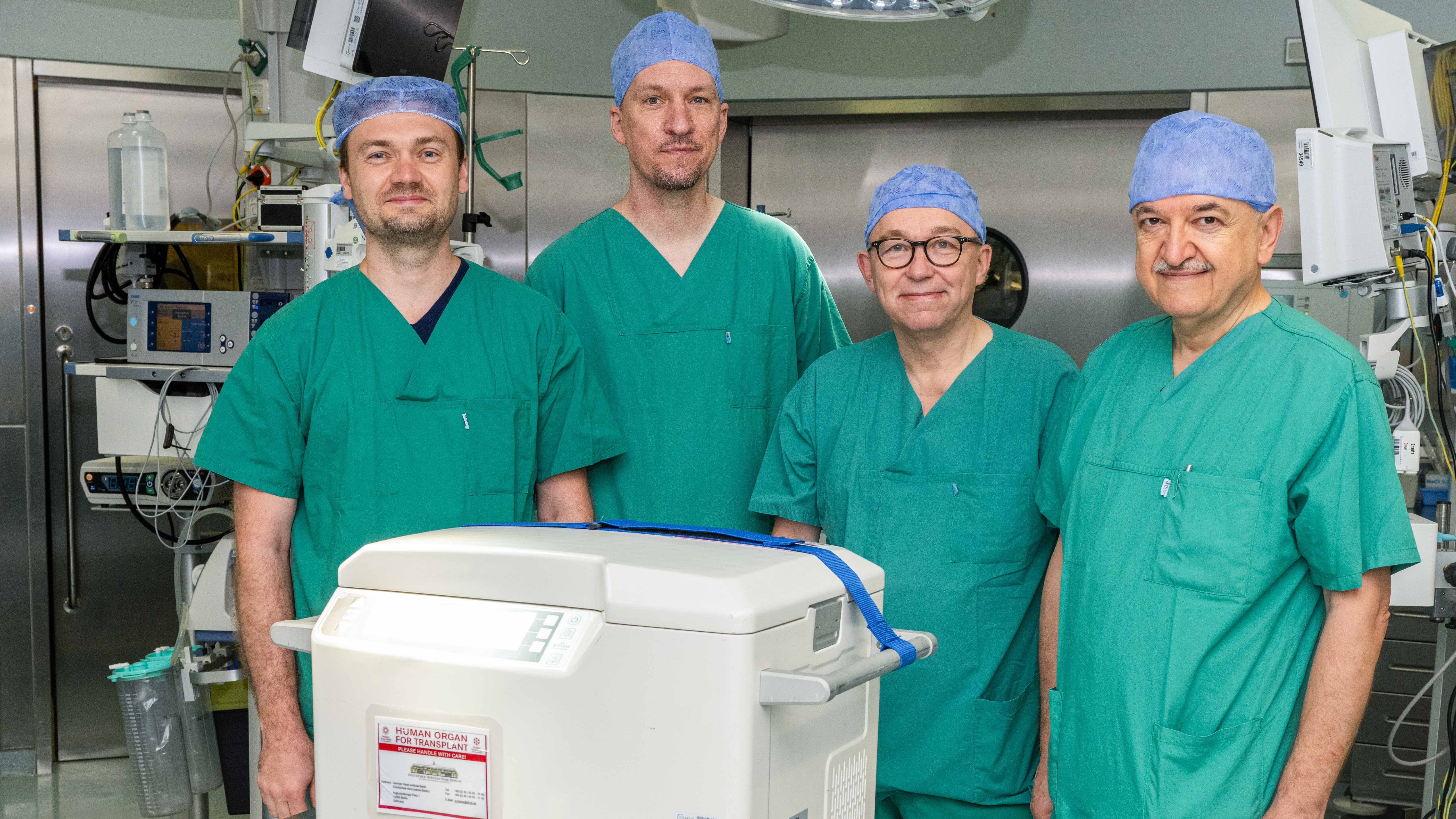
The system consists of a device, called the ‘XVIVO Heart Box’, for transport and a special solution for preserving the organ. Before transport, the device is filled with a newly developed nutrient and preservation solution. After removal, the donor heart is first connected to the circulating pump in the ‘Heart Box’ and then stored floating in the nutrient and preservation solution. During transport, the organ is continuously supplied with fresh oxygen. This circuit is cooled to a constant eight degrees Celsius for additional preservation of the organ.
The Berlin scientists involved in the study (from left): Leonhard Wert MD, Felix Hennig MD, Prof Christoph Knosalla MD and Ruhi Yeter MD from the DHZC Clinic for Cardiac, Thoracic and Vascular Surgery.
Outlook: Xenotransplantation
Animal organs as a future prospect
Xenotransplantation refers to the transfer of animal organs - primarily from pigs - to humans. Intensive research is being conducted into this technology worldwide, as it has the potential to significantly reduce the organ shortage in the long term.
Current developments
Since 2022, pig hearts and pig kidneys have been successfully transplanted into critically ill patients for the first time in the USA. The survival times documented to date range from up to two months after a heart transplant to four months after a kidney transplant.
The organs used come from genetically modified pigs, whose genetic material has been specifically altered to reduce immune reactions and acute rejection processes and to eliminate potential viruses.
These advances show that animal organs can in principle be made ‘compatible’ with the human body.
Chances of xenotransplantation
The technology harbours enormous potential:
- In future, organs could be available in a planned and needs-based manner.
- Waiting times would be significantly reduced.
- Seriously ill patients could be helped faster.
Risks and current status in Germany
Despite promising results, xenotransplantation is still at the experimental stage. The most important challenges include
- rejection reactions, which can occur despite genetic adaptations
- Possible transmission of unknown animal pathogens
Due to these risks, xenotransplantationis not authorised inGermany. Strict legal requirements - including those from the Transplantation Act (TPG), the Infection Protection Act (IfSG) and the Genetic Engineering Act (GenTG) - currently rule out clinical applications.
Nevertheless, intensive research is also being carried out in Germany.


