Before the heart transplant
For patients with severe heart disease, a transplant is often the last hope. At the German Heart Center of the Charité (DHZC), we have been performing heart transplants for almost 40 years and provide our patients with intensive care before and after the transplant - for the rest of their lives.
We are one of the leading German centers for heart and lung transplantation. As a supra-regional center, we care for patients from all over Germany. In total, over 3,000 thoracic transplants have already been performed at the German Heart Center at Charité. This makes the DHZC the largest center in Europe.
Our experienced and multidisciplinary teams specialize in the diagnosis and treatment of so-called terminal heart diseases that require a transplant. Cardiologists, pulmonologists and cardiothoracic and vascular surgeons work hand in hand with nursing staff, nutritionists and psychologists to ensure that patients receive individualized care.
Indication
Who is eligible for a heart transplant?
A transplant is the best possible treatment alternative for patients with serious heart conditions. On the one hand, this increases the patient's chances of a high quality of life in the long term; on the other hand, it is a complicated operation that can lead to considerable physical and emotional stress.
A heart transplant may be necessary for patients with these diseases, among others:
Severe (terminal) heart failure based on:
- cardiomyopathies - congenital, acquired and metabolic cardiomyopathies
- Myocarditis - inflammation of the heart muscle
- Severe congenital heart defects, such as Fontan circulation
- Life-threatening, untreatable arrhythmias
However, a heart transplant is only an option if:
- all other medical, interventional or surgical therapies have been exhausted
- life expectancy with the diseased heart is significantly limited
- those affected are in a “terminal stage” of the disease
- there are no serious concomitant diseases that would make transplantation impossible.
As the heart and lungs are closely connected via the blood circulation, diseases of one organ can also cause impairment of the other organ. If both organs are damaged, a heart-lung transplant is performed if possible.
Early medical clarification is crucial. We are happy to advise patients and their treating physicians on whether a transplant is an option.

Who gets a donor organ?
An organ transplant is only possible if there is no other promising therapy to treat the disease. As there are too few suitable donor organs, strict criteria apply to the allocation. The decisive factors are primarily those that make a transplant urgently necessary and increase the chances of success of the procedure.
Whether a patient is eligible for a transplant is decided by the treating physicians according to globally valid guidelines. For example, patients suffering from malignant tumors or other serious illnesses are excluded from a transplant.
If a patient is eligible for a transplant, an active listing with Eurotransplant can take place. Eurotransplant allocates organs according to the following criteria:
- Matching blood group
- donor and recipient are as similar in height and weight as possible (+/- 15 percent)
- Furthermore, the urgency is taken into account according to the severity of the clinical picture.
The waiting time can vary significantly from patient to patient and can take up to several years;
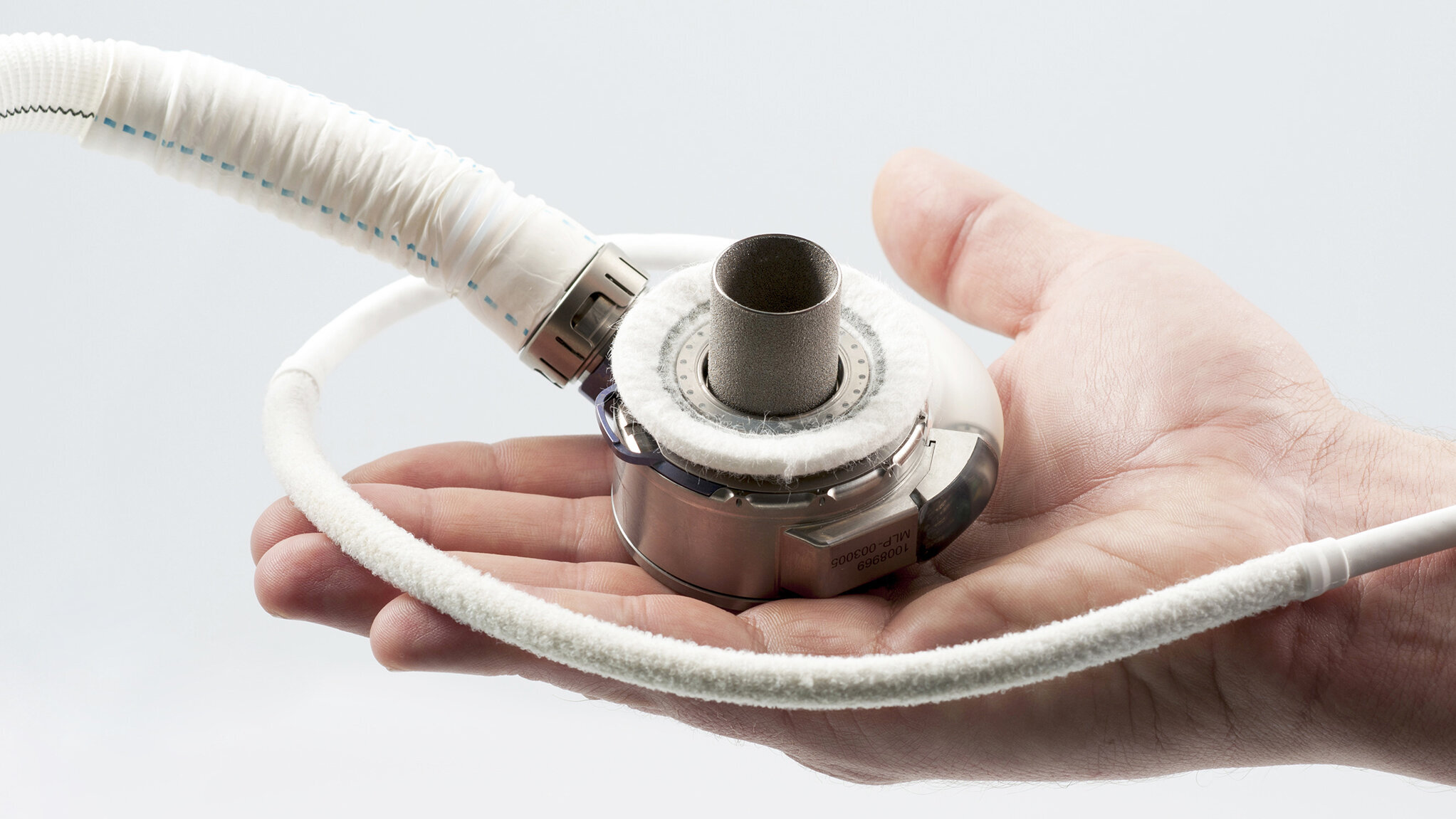
Patients with acutely life-threatening and incurable heart failure for whom a donor organ is not available in time are therefore often given an artificial circulatory pump. These systems are called VAD (“Ventricular Assist Device”) or also artificial heart systems and consist of a small pump that the doctor inserts directly into the patient's heart
Thanks to improved techniques and surgical procedures, artificial heart systems are increasingly becoming a longer-term alternative to transplantation.
Diagnostics
In order to decide whether a patient requires a heart transplant, we carry out a multimodal, very comprehensive diagnostic program. At the DHZC, we carry out these examinations, among others:
- echocardiography
- Cardio-MRI
- Cardiac catheter examinations
- Spiroergometry to measure physical resilience
- Computed tomography (CT)
- Long-term ECG
The assessment also includes the function of other organs (e.g. kidney and liver), blood markers and inflammatory values as well as the immune status. Other criteria include whether the patient requires a mechanical circulatory support system and whether they have had to be treated repeatedly in hospital in the past.
For the overall assessment of whether a patient is a candidate for a heart transplant, the following are also required:
- Psychological / psychosocial assessment
- Infectiological diagnostics
- Tumor screening
- Examination of the dental status
- Checking the vaccination status
Psychological support
A heart transplant is a serious procedure that is also psychologically stressful and challenges the emotional coping skills of all those affected. In order to provide you with the best possible support, even if you are under psychological stress, the psychocardiology department at the DHZC offers all our transplant patients comprehensive psychotherapeutic support before and after the transplant, including lifelong outpatient aftercare if necessary.
In the run-up to a heart transplant, we routinely conduct preparatory and diagnostic discussions with all patients. If you wish, we can also accompany you after the operation during your inpatient stay at the DHZC. This offer also applies to close relatives of our patients.
Psychotherapeutic discussions can help our patients to maintain their emotional well-being and inner strength during the often lengthy treatment processes or waiting times for an organ offer;
Please contact us if you would like psychological support! You can reach us at psychokardiologie@dhzc-charite.de.
During an inpatient stay, please contact the doctors or nurses treating you on the ward or the doctors or nurses of your relatives. They will then pass the information on to us accordingly. For outpatient treatment at the DHZC, please contact your attending physician;
Organ donation and donor heart
Complete anonymity to protect your privacy
Important to know: In Germany (and similarly in many other European countries), in the case of a heart transplant, it is not disclosed from whom or where the organ comes from. Organ donation is anonymous. The name, origin and exact identity of the donor are therefore not disclosed. The donor's relatives also do not find out who receives the organ.
This regulation serves to protect the privacy of both parties, i.e. the donor's family and the recipient.
Anyone can digitally deposit their personal decision for or against organ and tissue donation either in the organ donor card or, since 2024, in the nationwide organ donation register.

As a potential organ recipient, you can also be registered for organ donation at the same time. This has no influence on organ procurement in the event of receipt;
Legal regulations on organ donation
Organ donation in Germany is regulated by the Transplantation Act. This law strictly separates the areas of organ donation, organ procurement and organ transfer in order to avoid conflicts of interest. The Transplantation Act forms the legal basis for organ and tissue donation. It came into force in 1997;
Since March 1, 2022, the “Act to Strengthen the Willingness to Decide” has been in force. It aims to promote and document the personal decision to donate organs. The aim is to improve education about organ donation and to inform citizens regularly about their options for example through the introduction of a nationwide online register, targeted information by GPs: information materials and firmly anchoring the topic of organ donation in first aid courses. The law is based on the decision solution: organs and tissue may only be removed if the deceased person consented to this during their lifetime. If there is no documented decision, the next of kin are asked.
The objection rule, on the other hand, is currently not permitted in Germany. In countries where this applies, every adult capable of giving consent is a potential organ donor unless he or she has expressly objected.
Donor organs are distributed by law via the non-profit Foundation Eurotransplant in Leiden, the Netherlands, and transport is organized via the German Organ Transplantation Foundation (DSO) German Organ Transplantation Foundation (DSO). The donor organs usually come from donors who have died of brain death from the eight participating countries of Eurotransplant (including Germany).
Organ donation after cardiovascular arrest (DCD)
In Germany, organs may only be donated after brain death. This is the complete, irreversible loss of all brain functions - the cerebrum, cerebellum and brain stem are irretrievably destroyed. Although the patient is still on a ventilator, he or she is medically and legally dead.
In many other European countries, organ donation after cardiovascular arrest is also permitted. This is referred to as Donation after Circulatory Death (DCD). In this case, organ donation is possible if the heart stops irretrievably and there is no longer any blood flow.
Forms of DCD
- In controlled DCD (cDCD), circulatory arrest occurs when life-sustaining measures are terminated in patients with a hopeless prognosis. After cardiac arrest, a fixed waiting period is observed before organ donation can begin. The advantage of this is that the procedure can be planned and the transplant team can be prepared.
- In uncontrolled DCD (uDCD), circulatory arrest occurs unexpectedly, for example after unsuccessful resuscitation in the emergency room or outside the hospital. If it is clear that a return to life is not possible, organs can be harvested according to established protocols. The advantage is that the number of donations can be significantly increased, even if the procedures have to be carried out very quickly.
Differences to brain death
- In the case of organ donation after brain death, the patient is still artificially ventilated. The organs remain well supplied with blood and the processes can be planned.
- In a DCD donation, the organs must be secured very quickly after circulatory arrest because they can be damaged without blood flow.
Experiences in Europe
- In Spain, both controlled and uncontrolled DCD is carried out. Around a third of all donors today come from this group.
- France has established uncontrolled DCD, particularly in large cities.
- Controlled DCD has also been introduced in the Netherlands, Belgium, the UK and Switzerland. This has led to a significant increase in donor numbers.
Conclusion
Organ donation after cardiac arrest (DCD) is an additional procedure that is successfully used in many countries to help more patients on waiting lists. In Germany, this procedure has not yet been approved by law - but the discussion about it is becoming increasingly intense.
Requests for heart transplantation
At the DHZC, patients receive comprehensive care before and after a heart transplant in our “University Outpatient Clinic for Transplantation Medicine”. The first contact with us is usually made by your attending physician. The listing process begins with the request. After a detailed diagnosis, we plan a possible listing together. You can find out more on the page “Before heart transplantation”.
For the first step, we ask you to provide the following data, information and findings:
- Registration form
- Doctor's letter
- Details of the diagnosis
- Information on cardiac function
- Resilience
- Concomitant diseases
- Other relevant findings
This data is important for us to be able to assess the type and urgency of the transplant. If necessary, we will ask you for further information. The documents can be submitted by e-mail, fax or post.
We will then arrange an appointment with you for your first consultation. You will need the following documents for this outpatient appointment:
- referral
- Health card (insurance card)
- Vaccination card
- Absolutely necessary: Your medication plan (standardized medication plan according to § 31a in SGB V, available from your family doctor)
Optional (if available):
- Findings of the last cardiac catheterization or cardiac MRI examination (on a data carrier incl. written findings or via upload portal)
- CT findings (on a data carrier incl. written findings or via upload portal)
- If applicable, further documents (ultrasound of abdomen and heart, findings of dentist and gynecologist, laboratory values)
- We do not issue transportation tickets. If necessary, please bring one with you for the outward and return journey.
During this appointment, we will carry out a selection of the following diagnostics:
- Taking vital signs, blood pressure, pulse, height, weight
- Determination of current blood values
- Echocardiography
- Spiroergometry
At the same appointment, we will then discuss the results with you and our assessment of a possible inclusion on the Eurotransplant list.
The necessary evaluation diagnostics to be organized with the family doctor will then be discussed;
Contact
Telephone availability of the outpatient clinic:
Monday - Friday 09:00 and 17:00
We prefer contact by e-mail.
For patients and doctors:
T: +49 30 4593 2141, +49 30 4593 2140
F: +49 30 4593 2143
Management and contact persons
Maren Godde and Dr. med. Laurenz Kopp Fernandes are the medical directors of the outpatient clinics at the DHZC Clinic for Cardiac, Thoracic and Vascular Surgery.
Heike Bettmann is the nursing manager of the transplant outpatient clinic at the DHZC. She and her team accompany patients before and after transplantation. As an experienced contact person, she coordinates procedures, looks after relatives and ensures that our patients feel that they are in good hands at all times.
Patients who have undergone a transplant at the DHZC are automatically treated in our heart transplant outpatient clinic after discharge from hospital. Our experienced team will contact you to arrange regular check-ups. Our doctors and nurses in the outpatient clinic will also be happy to answer any acute questions or problems you may have.
Patients who have received their donor heart at another clinic and would like to transfer to the DHZC transplant outpatient clinic are also welcome to contact us. We will check your documents and findings and will be happy to arrange an appointment with you after consultation with the transplant center.
Telemedical treatment
We also offer our patients telemedical services as part of their aftercare - to manage their therapy at home. In contrast to face-to-face medicine, telemedicine overcomes the physical distance between patient and therapist with the help of telecommunications (e.g. mobile phone or internet).
We equip patients with digital measuring devices so that they can transmit their measurements to us wirelessly and easily from home - every day. Our experienced specialists from the outpatient clinic check these readings and, if necessary, contact you or your treating doctor immediately. The costs for telemedical co-care are covered by your health insurance.
Checklist for your first appointment in our outpatient clinic
Various documents are required for registration at the outpatient clinic. Please bring these documents with you to your appointment at our outpatient clinic:
- Referral
- Health card (insurance card)
- Your medication plan (it is best to ask your family doctor beforehand)
- Your vaccination card
- Any other documents requested by us, such as ultrasound of the abdomen and heart, findings from the dentist or laboratory results
Diagnostics
During your appointment in our outpatient clinic, we will carry out a selection of the following diagnostic tests in addition to the nursing admission:
- Taking your vital signs, blood pressure, pulse, height, weight
- Determination of specific blood values relating to the transplanted organ, the immunosuppressive therapy and possible effects on other organs in the body such as the liver and kidneys
- Echocardiography
Contact
Telephone availability of the outpatient clinic:
Monday to Friday: 7.30 am - 4.00 pm
We prefer contact by e-mail.
For patients and doctors:
T: +49 30 4593 2141, +49 30 4593 2140
F: +49 30 4593 2143
Additional doctor-doctor contact by e-mail.
Management and contact persons:inside
Maren Godde and Dr. med. Laurenz Kopp Fernandes are the medical directors of the outpatient clinics at the DHZC Clinic for Cardiothoracic and Vascular Surgery;
Heike Bettmann is the nursing manager of the transplant outpatient clinic at the DHZC. She and her team accompany patients before and after transplantation. As an experienced contact person, she coordinates procedures, looks after relatives and ensures that our patients feel that they are in good hands at all times.


